Owen used to run faster than 490 meters per minute. The highest he ever jumped was 4 feet, 6 inches. But then he got hurt.
Owen is a 13-year-old horse. The injury happened last fall in Woodside, Calif. while he was competing in an equestrian competition, galloping over fixed obstacles during the cross-country phase.
“We believe he hyperflexed his leg and tore his superficial digital flexor tendon,” says his owner, Simone van Ommeren-Akelman, a UC Davis student on the equestrian team.
But Owen is far from finished. For treatment, van Ommeren-Akelman chose UC Davis, believing Owen would have the highest chance of rehabilitating properly under the care of Dr. Larry Galuppo. Galuppo is a professor and chief of equine surgery with a focus on using regenerative medicine techniques — e.g. stem cell therapy — to treat musculoskeletal injuries.
During the fall of 2015, Galuppo treated Owen in the veterinary school’s Large Animal Clinic. He harvested stem cells from Owen’s sternum and twice injected them into the injured tendon, and into the artery in his leg once. Before van Ommeren-Akelman bought him four years ago, Owen suffered a similar injury, but she says the previous owner didn’t use stem cells. With this approach, Galuppo hoped to address both the old and new injuries.
And Galuppo believes athletes might learn some things from horses: Think about football players who suffer neck injuries, a sprained hamstring or a torn ACL. These types of injuries can derail careers. For this reason, he and the veterinary school have teamed up with the UC Davis School of Medicine to propose a series of parallel clinical trials. The goal? To see how regenerative technology used on horses can be applied to athletes with similar injuries.
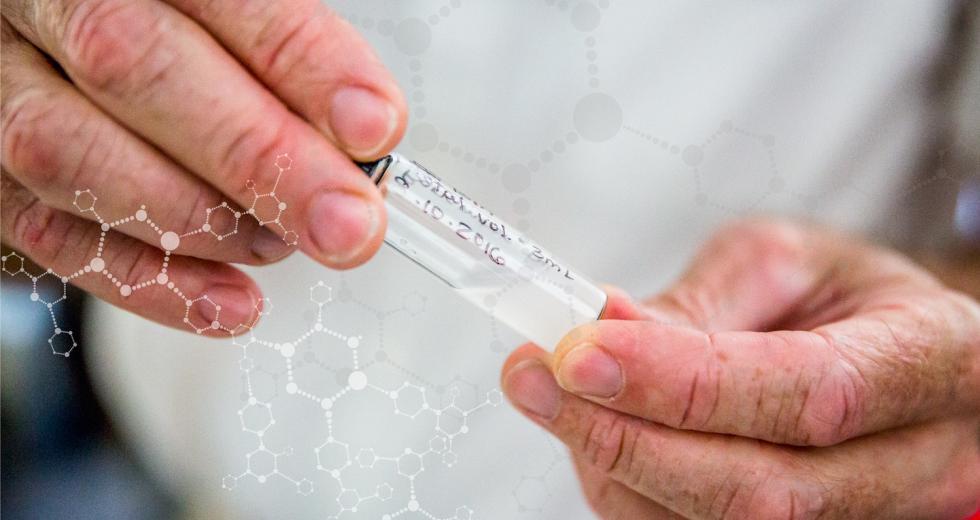
Larry Galuppo (far left) explains an ultrasound procedure to the
owners of one of the horses participating in a stem-cell clinical
trial at the UC Davis Veterinary Medical Teaching Hospital.

“When we’re treating tendons, ligament injuries in racehorses and jumping horses, many of those injuries cross over to what they’re treating in soccer, football and baseball players,” Galuppo says. “A horse is more likely to injure his stifle, which is similar to the human knee, similar to what might be seen in a football player who makes a wrong turn on the AstroTurf.”
The group recently submitted their proposal to the university’s Big Ideas program. In the coming months, they will meet with key stakeholders to gauge the level of interest and potential support. The university plans to make its final decision next summer. The Food and Drug Administration doesn’t approve of stem cell treatments on humans because there is limited evidence to back up their effectiveness. With the industry unregulated, many researchers and physicians claim stem cell therapy is unproven and potentially dangerous. Years ago, the high-profile stem cell clinics were in Europe, and athletes flew overseas to get the injections. These days, hundreds of clinics across the country offer treatments to patients — with no official standards in place.
Galuppo says that could change if the university gets the greenlight.
BANK SHOTS
Regenerative therapies are still a relatively new, unknown field in sports medicine. Only in the past five to seven years has it really taken off, says Dr. Melita Moore, head team physician for the UC Davis Aggies teams and an assistant professor in the Department of Orthopaedics.
Initially, doctors were performing autologous blood injections, which draw blood out and inject it back into tendons, ligaments and muscles to see if the injury will heal. That evolved into platelet rich plasma therapy, which uses platelets from the athlete’s own blood to treat inflammation and soft tissue injuries.
Related: Opportunity of a Lifetime
Moore believes UC Davis could be the first institution in the country to have an approved clinical trial using banked stem cells in a young, athletic population. The concept could take time to catch on. Getting an injection of someone else’s stem cells might seem different from your own, but Moore says this would be no different than any other donation system.
“Think about if you had to go to the hospital and get a pint of blood,” she says. “It’s that same concept, except you don’t have to match anything because a stem cell is just a blanket cell.”
But the use of stem cells has been controversial since the beginning. Should stem cells be regulated as a drug? Or should they be judged differently because the cells used for injections come from the patients’ own bodies? What if they were to come from someone else’s body? Many athletes pay no mind to these questions.
“Athletes are going to Germany, Korea and other offshore clinics, paying tens of thousands of dollars, and we have no idea what they’re getting,” Moore says. “It’s unregulated. We don’t have the clinical data to be able to support its use, quantify the healing response, prescribe the correct rehabilitation protocol, etc. because it’s not well-studied.”
This is why a trial is so critical. Currently, UC Davis does not offer stem cell treatments to its patients or athletes. But the clinical trials they are pursuing using their Good Manufacturing Practice facility could help prove if and how this type of therapy works — and transform the use of regenerative therapies in the world of sports medicine, Moore says.
BLANKET CELL
A “blanket cell” refers to a type of stem cell known as mesenchymal stem cells. These MSCs, which come from bone marrow, are elongated fibroblasts known for their ability to morph into various cell types depending on their location: bone cells, cartilage cells, fat cells.
“When we’re treating tendons, ligament injuries in racehorses and jumping horses, many of those injuries cross over to what they’re treating in soccer, football and baseball players.” Dr. Larry Galuppo, chief of equine surgery, UC Davis Veterinary School of Medicine
In horses and humans, the hip is a prime site for MSCs. Because it contains a large marrow, doctors can draw a significant volume without causing any negative effect for the donor, according to Dr. Fernando Fierro, assistant adjunct professor with the stem cell program at UC Davis Health System.
MSCs account for only about one in 100,000 of the various cells in bone marrow. But MSCs can multiply extremely fast in the right conditions. Fierro puts extracted marrow in a sterile plastic flat bottle, called a tissue culture flask. He then places the flask in an incubator at 100 degrees Fahrenheit with carbon dioxide levels at 5 percent and oxygen levels at 1 to 5 percent.
In three to four weeks, as the other types of cells die off, MSCs double every day, growing to 1 million or more in what Fierro calls a “superdose of repair cells.” But these cells can’t grow forever. Unlike embryonic cells that have no time limit, MSCs can become old and stop dividing after a few months, so he usually keeps them in an incubator for no more than a month.
Fierro calls these cells “architects” in the sense that, when injected, they often don’t repair the damaged area by replacing the missing or damaged cells, but direct other cells to the injury. They promote new blood vessels to grow and reduce inflammation, he says. Fierro works mostly with human cells. Human bone marrow can be purchased from many different vendors, and many researchers obtain fresh or frozen marrow this way. Of course, horses and humans are different animals. But equine treatments offer better comparisons to humans than mice, which have tiny bones.
THE BEST OFFENSE
Jim Kovach used to run — his best time for the 40-yard dash was 4.8 seconds. But then he got hurt.
Kovach is a 60-year-old man. He was a 238-pound middle linebacker for the New Orleans Saints and San Francisco 49ers from 1979 to 1985. A ruptured ACL ended his football career, and stem cell therapy wasn’t an option at the time.
“In all frankness, had it been available and approved by FDA, I would have tried it,” Kovach says.
But Kovach was far from finished. With a medical degree from the University of Kentucky and a law degree from Stanford, Kovach started backing various startups and independent research institutes with a focus on regenerative medicine.
Related: Can stem cells grow the region’s bottom line?
“The idea was to develop therapies that were truly regenerative instead of just stop-gap approaches to treating sports injuries,” he says. “That was in the ‘90s. Sports medicine always lagged behind other areas.”
Jim Kovach, a former linebacker, had to give up his football
career due to a ruptured ACL.

Now Kovach is serving as a key advocate for UC Davis, using his experience to reach out to the stem cell industry and find sponsors to support the trials and researchers. He believes the clinical trials can provide a roadmap for how these therapies can be delivered in a safe, effective and efficient way.
These days, he still deals with his own physical constraints. For his 60th birthday, his kids got him a Garmin fitness tracker to help him monitor his steps, heart rate and calories burned. But his running days are over. He can still walk on a golf course, he says. He does a lot of cycling, either outdoors or at his house in Marin County, on a stationary bike while watching the Giants game.
“It’s amazing how quickly muscle atrophies,” he says. “That’s a real motivation. Even in my own hip and other joints, if I haven’t worked out, I have to get home and get on my bike. If you don’t exercise, you’re going to lose it. That’s how skeletal muscle is. It’s a blessing and a curse.”
STEPS TO RECOVERY?
The parallel clinical trials would help answer some crucial questions about stem cell therapy: Where is the best place to put the cells? Should they be delivered directly to the damaged site or injected into the bloodstream? How long do cells last after being transplanted?
“These questions seem to be extremely relevant, but we don’t have the answers,” Fierro says. “There is a robust body claiming they’re safe and they don’t seem to be causing more damage. But how much are they helping? We still need to do a controlled trial to find out.”
Fierro says the only reason there has been no scandal to this point is because there has been no major stem cell catastrophes. But he understands the “drug or no drug” debate.
“Of course the doctor many times will use one part of the body to repair another part,” he says. “But in this case, you’re manipulating the cells a lot. It’s hard to argue that you are putting something back that was yours anyway, so there is some risk there.”
Kovach doesn’t recommend athletes look to unregulated therapies at stem cell clinics. He wants athletes to have solid research and actual results to back up the treatments and he feels optimistic about future developments at UC Davis. Galuppo does too, but he emphasizes that the clinical trials are just one step toward recovery from injury.
“There’s no miracle cure for musculoskeletal injuries,” Galuppo says. “We are using regenerative medicine therapies to help heal injuries and reestablish normal strength and function. Stem cells are just one of the many novel biological tools that are being used to enable athletes to return to full function.”
The tool seems to be working for Galuppo’s equine patient. For the first six months after the injections, Owen started walking 20 minutes each day, and van Ommeren-Akelman iced his leg twice daily, wrapping it at night. By summer, Owen was walking for an hour a day and trotting for 11 minutes.
“We are nine months into rehab,” van Ommeren-Akelman says. “He’s doing phenomenally. We think he’s going to make a full recovery.”
Recommended For You

Stemming Out
UC Davis researchers deliver lab innovations
Dr. Jan Nolta is a whirlwind of energy, and this July morning she is blitzing through UC Davis’ brand-new Institute for Regenerative Cures, a state-of-the-art lab where scientists and researchers are working on breakthrough discoveries and stem cell therapies.

Unnatural Selection
Scientists at UC Davis may be on the cusp of an HIV cure
The person who finds the cure for HIV will have their name etched in medical history. It’s a hard pill to swallow for one man who has spent 40 years chasing a cure. A cure for HIV, built upon decades of his work, could very well be proven this year. Yet Dr. Gerhard Bauer’s name may be little more than a footnote in the arcane medical journal that publishes the breakthrough.
This is the story of curing HIV.