Too many pregnant mothers know the feeling of horror: The ultrasound reveals something wrong. Perhaps it’s nothing. But maybe it’s life-threatening, a disease or a disability. Maybe it’s the unthinkable. For hundreds of thousands of years, the unthinkable — babies doomed to die or develop impairments before drawing their first breath — meant only tragedy and heartache.
Now there is hope. Surgeons at UC Davis Medical Center in Sacramento will soon begin performing fetal surgery, a procedure during which a baby is removed from the womb, treated and returned. The methods and technologies used build on work that began at the University of California San Francisco in 1981, where the “Father of Fetal Surgery,” Dr. Michael Harrison, first inserted a catheter to remove a blockage in the urinary tract of a child in utero, two weeks before its birth. Since then, Harrison has groomed a team of surgeons who have changed the face of fetal surgery and saved hundreds of lives.
“The idea of going beyond surgery and going to a gene level and wiping out a lifelong problem … it’s kind of sci-fi stuff, really.” Dr. David Schrimmer, chief of maternal-fetal medicine, UC Davis Medical Center
Many of these key players are coming to Sacramento. One of the pillars of the trailblazing UCSF team, Dr. Diana Farmer, joined UC Davis as surgeon-in-chief at UC Davis Children’s Hospital and chair of the Department of Surgery. She recruited another UCSF notable, Dr. Shinjiro Hirose, a nationally recognized children’s cancer surgeon and an expert in the development and use of surgical robotics in children. Hirose will serve as chief of pediatric general, thoracic and fetal surgery. They’re joined by Dr. David Schrimmer, the chief of maternal-fetal medicine and former professor of obstetrics and gynecology at UC San Diego, where he was the founding director of the UCSD fetal surgery program.
How did this all get started? And what, exactly, happens in a fetal surgery center? What are the risks? The surgeons gave us a tour.
The Breakthrough
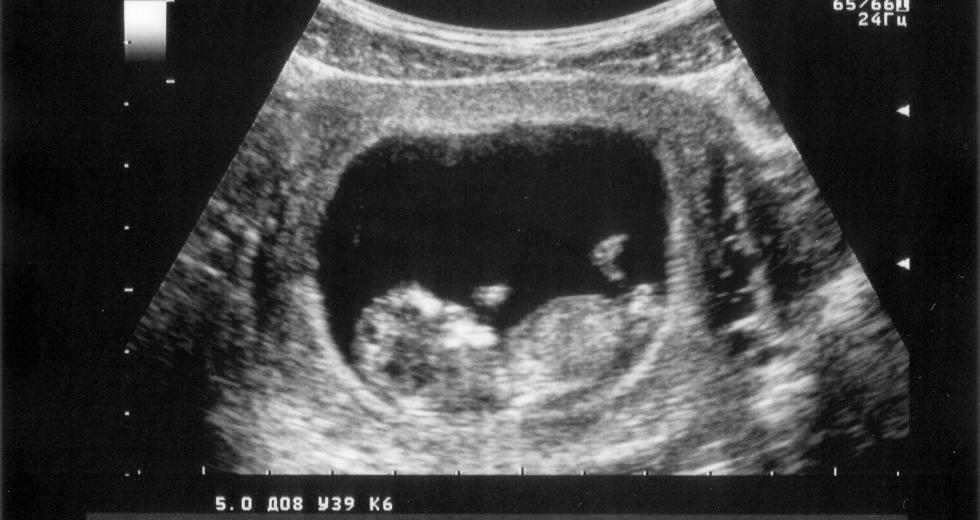
It started with the ultrasound. Before this game-changing imaging was available, doctors could do little more than wonder what was happening inside this “black box, otherwise known as the uterus,” Schrimmer says. “Everything was a surprise. Is it a boy or a girl? Does it have heart disease? Down syndrome? Spina bifida?”
The ultrasound gave doctors knowledge. That knowledge offered an opportunity to treat certain problems in advance. In some cases, this means fetal surgery, where the mother’s womb is opened, the fetus is removed from her body, operated on and then neatly tucked back into the uterus. “You never cut the umbilical cord,” says Hirose, who, like Farmer and Schrimmer, has performed more than 100 fetal surgeries. “The fetus has to stay connected to the umbilical cord; that’s the trick. That’s the challenge — to keep the pregnancy intact while we’re operating.”
There’s little question these procedures have saved lives. In addition to blocked urinary tracts, fetal surgery has proven effective at treating spina bifida, tracheal occlusion, diaphragmatic hernia and what is called “twin-to-twin transfusion syndrome,” a condition in which twins share a placenta and one twin effectively steals blood from the other. Without surgery, there are typically one of two outcomes: One of the twins dies or, 90 percent of the time, both of the twins die.
This math changed in 1997 when doctors at Vanderbilt University Medical Center performed the first in-utero surgery to save a twin. Surgeons are now able to use lasers and a fetoscope — a long, thin tube with a 3-millimeter diameter — to locate the twins’ umbilical cord and fix the problem.
“You go in with the scopes, and you find the umbilical cord of one twin, then find the umbilical cord of the other twin, and you can trace them backwards to the placenta, like a bowl of spaghetti,” says Schrimmer. “You look for the blood vessels that don’t stay in ‘their half’ of the placenta. Once we find them, then we zap them — sort of like a video game.”
This prevents the theft of blood from one twin to the other, restoring the normal 50/50 share. Thanks to this type of intervention, that 90 percent death rate has been flipped to an 80- to 90-percent chance of at least one twin surviving. These tiny scopes, nearly microscopic, also give new ways to treat babies starved of blood.
Drs. Diana Farmer, Shinjiro Hirose and David Schrimmer are
leading the new Fetal Surgery Center for the UC Davis Health
System.

“In conditions where the baby is anemic and needs blood, you can take a fine needle and put it in the umbilical cord, paralyze the fetus so it doesn’t move and actually give it a blood transfusion through the needle,” Schrimmer says.
The Test
Each year, there are 4 million babies born in the United States. About 2,000 are born with spina bifida, Latin for “split spine.” In the condition’s most severe form, myelomeningocele, the spinal cord juts out of the spine, forming a sac above the skin. This can cause paralysis, bowel dysfunction, nerve damage, learning disabilities and tendonitis. No one knows what causes it. There is no cure.
Historically, spina bifida was only treated after birth, when the doctors could patch the hole in the spine. At UCSF, Farmer was a leading voice who asked, OK, but what if we can treat it sooner? What if we repair the spine before the baby is even born? This was not without controversy. While spina bifida is an awful condition that can terrify parents and hobble a childhood, it is not necessarily life threatening. The decision isn’t black and white. “In any operation we do on the fetus, the mother takes all the risk to herself, without a medical benefit,” Dr. Farmer says. “It’s similar to a liver transplant for a relative, where a healthy person undergoes a procedure for the benefit of someone else.”
She also adds that unlike a liver transplant, of the more than 1,000 fetal surgeries performed, no mothers have died. While fetal surgeries do require a caesarian for all future pregnancies, the risk of death itself, to this point, has been theoretical.
In the data-driven world of medicine, you don’t just whip up a new treatment and establish it as the status quo: you test it. You must prove that in a controlled, measured experiment, Treatment A is more effective than Treatment B. The results must be repeatable. Sometimes this is straightforward; if you want to test the efficacy of Advil to treat headaches, you simply give Group A the Advil, then you give Group B some sugar pills as a placebo. But a test for fetal surgery to treat spina bifida?
For that, Farmer helped lead the complex, $22.5 million Management of Myelomeningocele Study, which spanned eight years and a network of hospitals across the nation. They had to somehow ensure that a homogenous control group would not receive fetal surgery, and then compare their outcomes with mothers in San Francisco, Philadelphia and Nashville who did receive the surgery. “This study was a one-of-a-kind,” says Dr. Hirose. “To standardize the operation of the mother and the fetus and then standardize the follow-up. … It was extraordinarily difficult.”
“Every single thing we do generates an ethical conversation; you can see many sides to the arguments. None of the decisions are made in a vacuum.” Dr. Shinjiro Hirose, incoming chief of pediatric general, thoracic and fetal surgery, UC Davis Medical Center
They pulled it off. Over eight years, roughly 80 mothers with babies who had myelomeningocele had the fetal surgery, and a control group of 80 mothers (also with babies who had myelomeningocele) waited until after pregnancy. The results? The fetal surgery was so successful, they shut down the test two years earlier than planned.
“For a young couple, finding out their developing child has a problem is one of the most devastating things that can happen,” Farmer says. “This landmark study offers real hope for improving the lives of children with spina bifida worldwide.”
Every mother lived. In fact, according to Farmer, the thousand or so babies who had fetal surgery to treat myelomeningocele tended to have superior motor function of the legs, were half as likely to need a shunt and were eight times as likely to have a normally positioned brainstem, according to study co-author Dr. N. Scott Adzick, who added that, 30 months after birth, “nearly twice as many walked without crutches or orthotics.”
Still, it’s no guarantee of complete healing. For babies who did not get the fetal surgery, only 21 percent were able to walk at age 2-and-a-half. For babies who did get the surgery, the number doubled. Glass half full: that’s a huge improvement. Glass half empty: it’s still only 42 percent. This did not go unnoticed by doctors like Hirose. “One of the things that attracted me to come to UC Davis is that even though the children did better with that operation, we didn’t completely cure the disease,” he says. “Now we’re back in the lab, looking to improve the operation.”
Enter the All-Stars
When Dr. Farmer performed fetal surgeries at UCSF, she noticed that many of her patients were from Sacramento and the Central Valley. “I thought, ‘Gosh, it’s crazy for so many of the patients to have to travel so far,’” Farmer says. “And it’s much larger than just the fetal portion of it. There’s a lot of things we want to bring to this area, ranging from the fetus all the way through adolescence. Our goal is to be complementary to the great surgeons and team already in place at UC Davis.”
The doctors all stress the importance of “the team,” and Schrimmer even used his own sports analogy. “I thought, ‘Whoa, this is like getting drafted by the Yankees!’ I’m now part of a team that’s going to take this to a whole new level. That’s what we’re doing at Davis — we’re literally at the cutting edge of the science. It’s very cool for UC Davis and the patients who live around here.”
Fetal surgery has a ton of moving parts, so it’s essential that everyone is on the same page. Each operation takes two surgical teams (one for the mother and one for the child), must be perfectly timed and is usually finished in less than 90 minutes. The traditional job functions become blurry. Technically, once the baby’s out of the womb, that’s pediatric surgery.
After birth at UC Davis Medical Center, babies are placed on
these neonatal tables, where a team of doctors and nurses can
focus on the newborn while the mother is still in the adjacent
operating room.

So who should actually perform surgery on the child, a pediatric surgeon or a neurosurgeon, because they’re operating on the spine? “The bottom line is … who cares. It takes the whole team,” says Schrimmer. That team also includes neonatologists; if a surgery results in a delivery five months in, you need an ace neonatologist to handle the unique demands of an ultra-premature baby. Other key players include radiology, anesthesiology, nurses, social workers and an ethics oversight committee. “Every single thing we do generates an ethical conversation; you can see many sides to the arguments,” says Hirose. “None of the decisions are made in a vacuum.”
UC Davis brings a broad range of resources. “One thing that’s unique about the Sacramento region is that it’s really one of two or three places in the country that has a world-class vet school, a world-class [maternal-fetal medical] school, as well as world-class business and engineering schools,” says Farmer. This is critical. New surgeries require new tools — tools that can be made by Davis’ College of Engineering. The veterinary school is just as important. “Animal research is a touchy subject, but with some of the biggest new developments in medicine, you want to test them in animal models before testing them in human beings.”
This research is bound to unleash new discoveries, new treatments and new ways to save lives. If we’re only now in the early chapters of fetal surgery, what could we see in five years, 10 years?
“As the safety profile for the mother improves and as we do more and more minimally invasive procedures, you might argue that almost any birth defect could be treated before birth,” says Farmer, citing the example of sickle cell disease. And it’s a good bet that we’ll soon be hearing much more about stem cell treatment. “We have a bioengineering laboratory, and we’re looking at the application of stem cell therapy before birth,” says Dr. Farmer.
That dovetails with the vision of The University of California Fetal Therapy Consortium (Hirose is one of the group’s creators) a partnership of the University of California at San Francisco, L.A., Irvine, San Diego and Davis.
“We managed to collectively put our egos aside and say, it’s really dumb to be competitors, we should be collaborators. We should do cutting-edge new things,” says Schrimmer. Just weeks ago, the Consortium agreed to apply to the FDA for animal experimentation involving stem cells. “The idea of going beyond surgery and going to a gene level and wiping out a lifelong problem … it’s kind of sci-fi stuff, really.”
Ethicists can and will debate the pros and cons of stem cell research. But that’s not the job of the surgeons: Their mission is to push the science as far as they can, which, since the early days of Harrison, the father of fetal surgery, has unquestionably saved lives. And in this context, when they say “save a life,” they’re salvaging the entirety of a human life, from birth to age 80+.
As Farmer puts it, with fetal surgery, “You don’t just save a life. You save a lifetime.” She pauses, then jokes, “I try not to tell that to my geriatric colleagues.”
Recommended For You

Bedside Manner
Teacher Nicole Castles brings education to patients at UC Davis Children's Hospital
Nicole Castles teaches UC Davis Children’s Hospital in Sacramento. Castles is the sole instructor for all school-aged children in the pediatrics ward, as well as school-age patients in other wings of the hospital. In a given week she’ll schedule bedside sessions with as many as 30 students.

Brain-Powered Bionics
How technology is using mind control to help people walk again
There are 6 million people in the United States who are paralyzed. Wide-spread, thought-controlled medical solutions won’t be available tomorrow or next month or even next year. But what if, some day, all of those people could walk again?
Convenient Care
How concierge medicine is changing the health care marketplace
Think of your best friend, a friend that knows all your ticks, hobbies and vices. Now imagine this friend happens to be a doctor, and she’s your doctor.

Economic Regeneration
Can stem cells grow the region’s bottom line?
A broken leg used to be a death sentence for a horse. Now, the University of California veterinary teaching hospital in Davis is using stem cells to help the horses heal quickly.



Comments
Interesting article for Ash
Amazing and inspiring stuff!